Your Hemorrhoid & Rectal-Prolapse Surgeons
You’re not alone, nearly one in two adults
experiences haemorrhoids by age 50.
Persistent piles, fissures and prolapse all come from strain on the back-passage tissues. Piles are swollen veins; a fissure is a paper-cut-sized tear that bleeds and stings after a bowel movement ; prolapse means the rectum slips outside, causing mucus, bleeding or loss of control.
Soothing ointments ease itch but cannot shrink overstretched veins, relax the muscle spasm that keeps a fissure open, or tighten the weakened supports that let the rectum drop. When symptoms disrupt life, day-case surgery removes or staples piles, releases the tight internal sphincter so fissures heal, or hitches/staples the prolapsed rectum back inside without external cuts. The result is predictable pain relief, restored bowel control and a quicker return to normal activities.
What is an anal fistula?
An anal fistula is a narrow tunnel running from the skin near the back passage and opening into the anal canal higher up. This discharges pus irregularly and may be uncomfortable. It often shows up after there has been an abscess near the back passage.
What does the operation consist of?
The fistula has its roof cut away converting it from a tunnel into a trench. The trench becomes shallower as it heals, and ends up as a flat scar after a month or two.
What is an anal fissure?
An anal fissure is a small tear running from the skin near the back passage and opening into the anal canal higher up. This is a painful condition usually associated with fresh bleeding after bowel actions.
What does the operation consist of?
The fissure is aggravated by spasm of the circular anal muscle. This is stretched slightly and some of the muscle fibres divided. This results in relief of the spasm and thus the pain, allowing the fissure to heal. Any associated anal skin tags are removed.
What is the problem?
You have an abscess which has formed deep inside your tummy (abdomen). This is something brought on by infection after, for example, appendicitis, a burst ulcer, an operation or various other causes. The abscess is a pool liquid pus. It makes you feel ill and feverish. If left it can get worse and cause serious problems. Commonly these abscesses only show up two or more weeks after the infection. Also, they often need to be left even longer than this before they are ‘ripe’ enough to be opened up and drained safely. The abscess can form high up under the ribs, or deep down in the pelvis, or anywhere in between. Sometimes there are more than one.
What does the operation consist of?
A cut is made in the skin of the tummy as near as possible to the abscess. The cut is deepened until we hit the abscess. The pus then drains out to the skin. We put a drainage tube down into the abscess space to drain out any further pus. This tube stays place until it is clear from x‑ray tests that the abscess space is getting smaller. We can then shorten the tube, bit by bit. Finally the wound dries up and heals over.
What are piles?
Piles are the loose vascular (blood containing) cushions on the wall of the anal canal that may bulge out through the ring muscle (sphincter) which holds the back passage shut. They contain big blood vessels which may bleed with bowel actions or protrude out of the anal canal on straining. They can clot up when stuck outside causing pain. Prolapse can result in loose skin which may produce irritating tags.
What does the operation consist of?
The ring muscle is slightly stretched and the piles are trimmed off.
What is a Hydrocoele?
A hydrocoele is a pocket of watery liquid that has built up around your testicle. Sometimes this is because the testicle is diseased. More often it is because the liquid cannot drain into the circulation properly.
What does the operation consist of?
A cut is made into the skin over the hydrocoele. The liquid is emptied out. The testicle is examined. If it is all right the double coverings of the testicle are stitched up to stop the liquid building up again. If the testicle is diseased it may even be necessary to remove it. This will be discussed with you. Finally, the skin is stitched up.
If you suffer from chronic problems with a condition such as ulcerative colitis or familial adenomatous polyposis (F.A.P.), you may be advised that you must undergo surgery to remove the diseased bowel. This will usually mean having an ileostomy -the end of the small intestine is brought to the surface on the abdomen and a ‘stoma pouch’ is worn. Many thousands of people have ileostomies and have found that after the operation they enjoy a new improved quality of life -relieved of a constant preoccupation with bowel problems and reeling better than ever before.
Depending on your type of problem, however, you may be offered the option of having an ileo-anal ‘pouch’ instead of an ileostomy. This is where the diseased bowel is removed, but instead of bringing the end of the small intestine to the outside of your abdomen, a pouch is created internally (a little like a man-made rectum) and connected to the back passage, or anus. Waste matter, or faeces, can then be passed in much the same way as usual, although it will be more liquid and more frequent.
The pouch is not a perfect solution -no surgery will replace completely normal function of the colon and rectum -but for selected patients it can be an acceptable alternative to a permanent ileostomy.
What is the bowel?
The bowel is a tube of intestine which runs from the stomach to the back passage. It fits into your belly (abdomen) by coiling up in a loop. The upper part of the bowel is called the small bowel and it joins the lower part of the bowel (the colon) just to the right of the waistline. This is where the appendix pouches out from the colon. The colon runs up to the right ribs, loops across the upper part of the belly and passes down the left side to run backwards into the pelvis where it is called the rectum.
If the left side of the colon loop or the upper part of the rectum become diseased or develops a growth, this may cause crampy pains, diarrhoea, constipation, bleeding or a lump. The diseased part of the bowel has to be taken out and the ends are joined up whenever possible.
What does the operation consist of?
A cut is made in the skin of the lower abdomen in the midline about 30cm (12 inches) long. The left side of the colon and the upper rectum are freed from the inside of the tummy. The diseased part is cut out and usually the ends are joined together.
What is a Perianal Abscess?
This is an infection in the wall of the lowest part of the back passage. Pus builds up under the skin causing swelling and pain. There is sometimes a connection with the back passage itself.
What does the operation consist of?
The pus is let out through a cut in the skin. The wound is plugged with an antiseptic material. Sometimes antibiotics are given to help the healing.
What is a Pilonidal Sinus?
A pilonidal sinus is a condition caused by small hairs collecting under the skin between the buttocks. It is treated by removing the affected skin and involved tissue and closing the resultant defect with stitches. If there is associated infection or an abscess it may be dangerous to close the wound and it is then left open and allowed to heal up over a period of 4 to 10 weeks. The length of time taken for healing depends on the size of the wound. If the wound is left open it may require daily dressings initially. These will be arranged for you.
What is a rectal prolapse
The lowest part of the bowel, the rectum, in your case has become rather slack. When you strain, the lining of the rectum and finally the walls of the rectum pout out through the back passage (anus). As well as the pouting bowel, many people have soiling and cannot control the wind.
What does the operation consist of?
The aim of the operation is to hitch up the rectum stitch it to the inside of the pelvis so that it cannot pout out any more. Usually a nylon sheet is placed behind the rectum to help secure it. Sometimes the bowel may have become very slack and elongated which may require a section of the bowel to be removed . Over several months the loss of control of the wind and the soiling gradually get back towards normal.
What is a rectal prolapse?
A rectal prolapse occurs when the normal supports of the rectum become weakened, allowing the muscle of the rectum to drop down through the anus to the outside. Sometimes this only happens when you open your bowels, and goes back on its own. In more severe cases, the rectum may need to be pushed back after opening the bowels, or may even stay outside all the time.
While not a dangerous or life-threatening condition, this can be very uncomfortable, a considerable nuisance, and may cause loss of bowel control. There may also be a mucus or blood -stained discharge.
What is the bowel?
The bowel is a tube of intestine which runs from the stomach to the back passage. It fits into your belly (abdomen) by coiling up in a loop. The upper part of the bowel is called the small bowel and it joins the lower part of the bowel (the colon) just to the right of the waistline. This is where the appendix pouches out from the colon. The colon runs up to the right ribs, loops across the upper part of the belly and passes down the left side to run backwards into the pelvis where it is called the rectum.
If the right side of the colon loop becomes diseased or develops a growth, this may cause crampy pains, diarrhoea, constipation, bleeding or a lump. The diseased part of the bowel has to be taken out and the ends are joined up whenever possible.
What does the operation consist of?
A cut is made in the skin of the lower abdomen in the midline about 30cm (12 inches) long. The right side of the colon is freed from the inside of the tummy. The diseased part is cut out and usually the ends are joined together.
What is the bowel?
The bowel is a tube of intestine which runs from the stomach to the back passage. It is much longer than the inside of your belly (tummy) and fits in by coiling up in a loop. The upper part of the bowel is called the small bowel and it joins the lower part of the bowel (the colon) just to the right of the waistline.
The colon runs up to the right ribs, loops across the upper part of the belly and passes down the left side to run backwards into the pelvis towards the back passage where it is called the rectum. If most of the colon is diseased it can cause diarrhoea, bleeding or general illness. It is better removed.
Sometimes the ends can be joined up inside your abdomen. More often, the back passage is not healthy enough to make a safe join and then the lowest part of the small bowel is brought out as a sort of spout (ileostomy) on the right side of the tummy. The bowel waste runs into a special bag stuck over the ileostomy.
What does the operation consist of?
A cut is made in the skin of the abdomen about 25 cm (10 inches) long. The colon is freed inside your tummy. The diseased bowel is taken out and the lower end of the remaining bowel is stitched shut. The upper end is opened as an ileostomy. The wound in the tummy is stitched up.
Most patients walk out two hours later
Local block + tablets, not morphine drips.
Separate waiting area, no gowns in corridors.
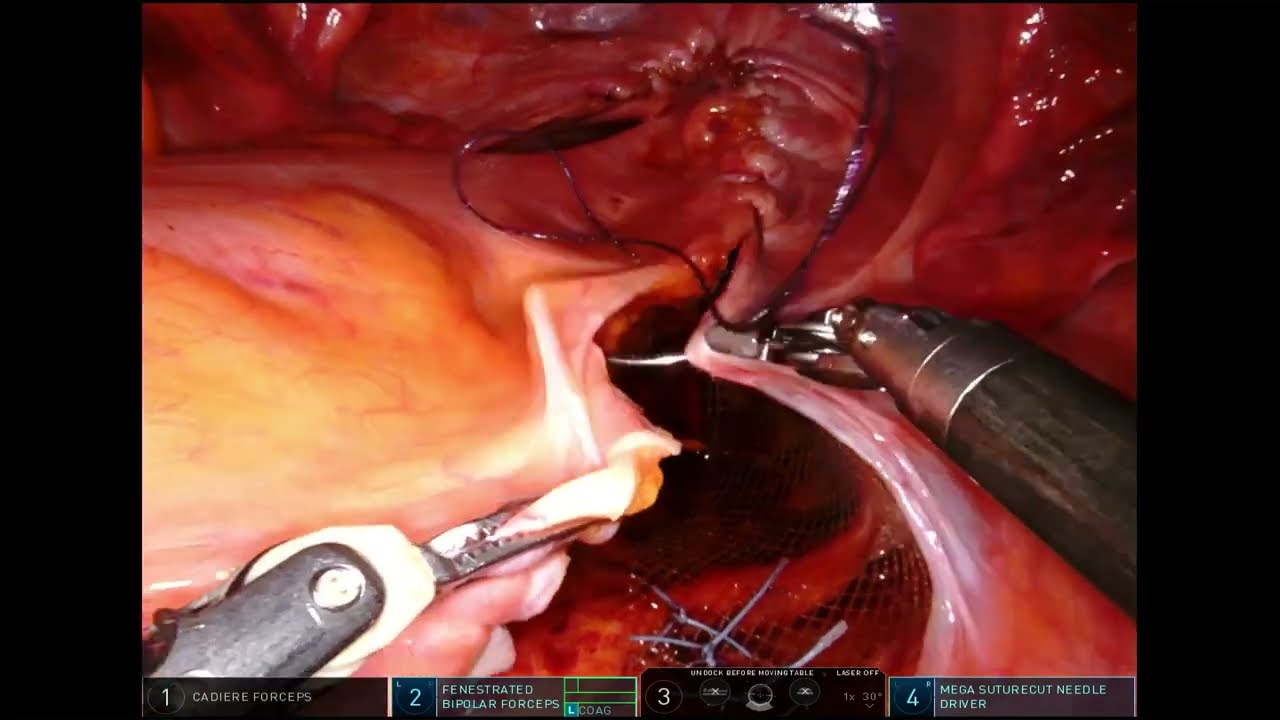
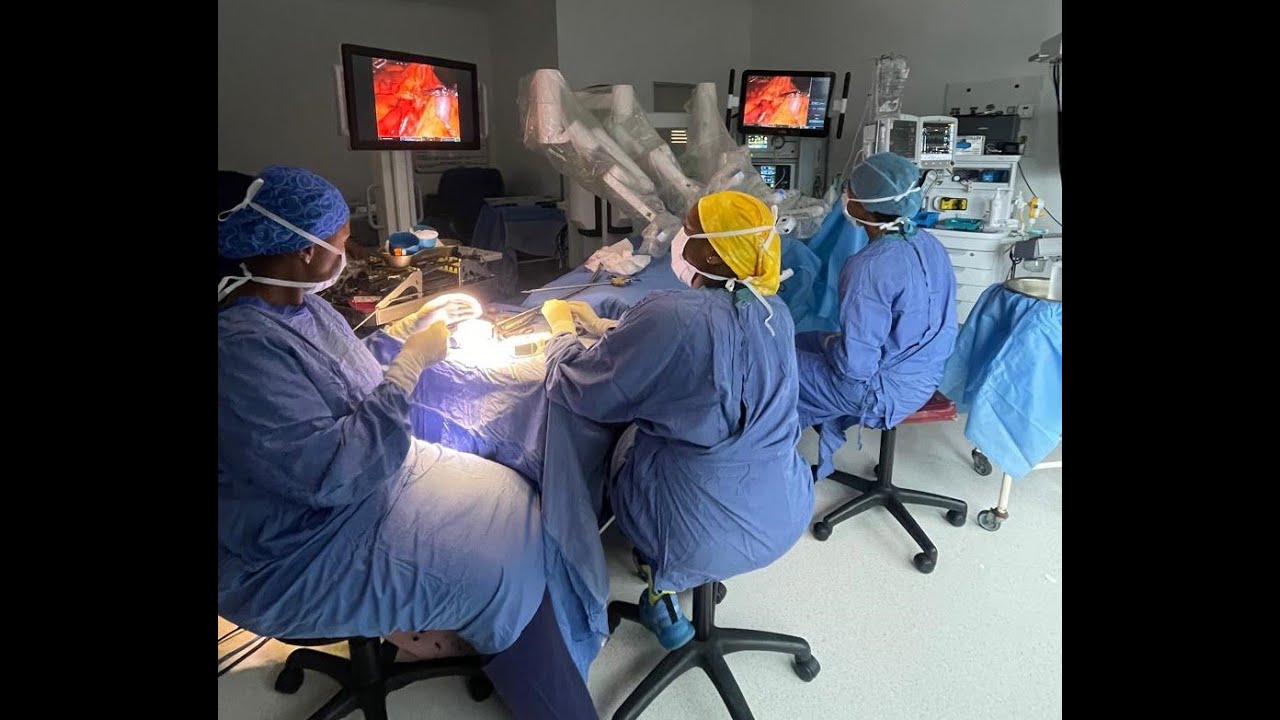
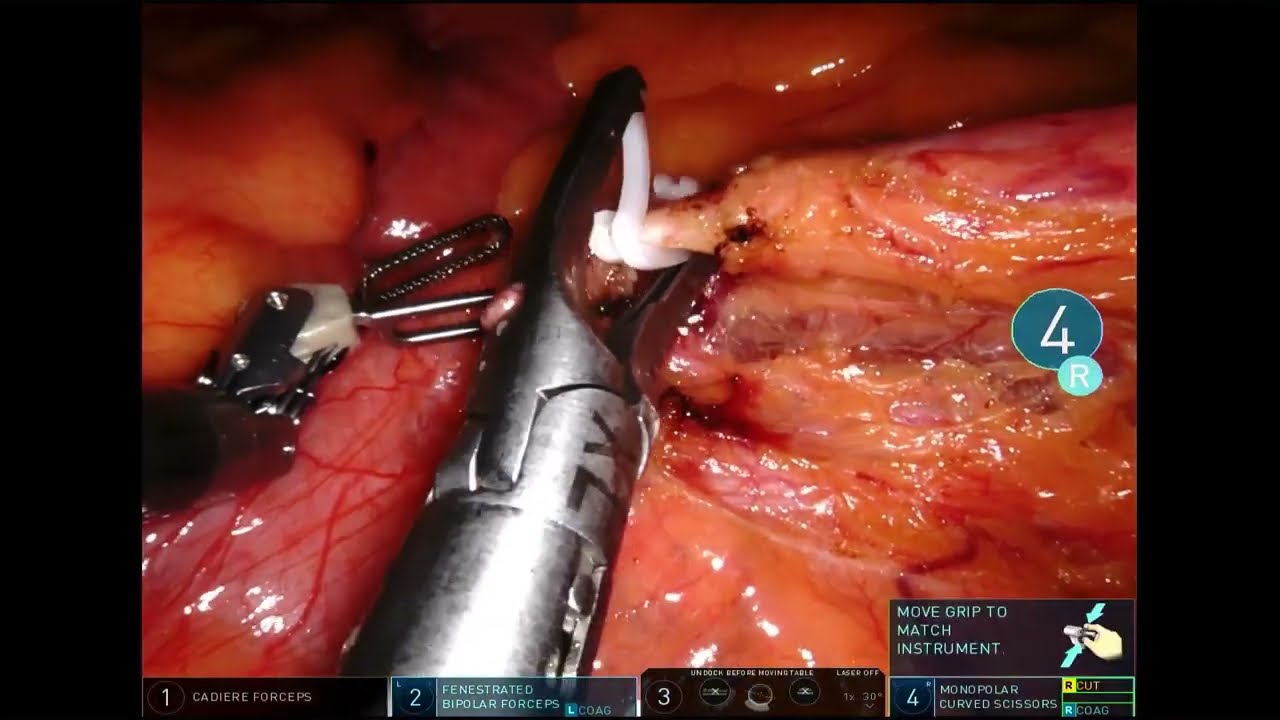
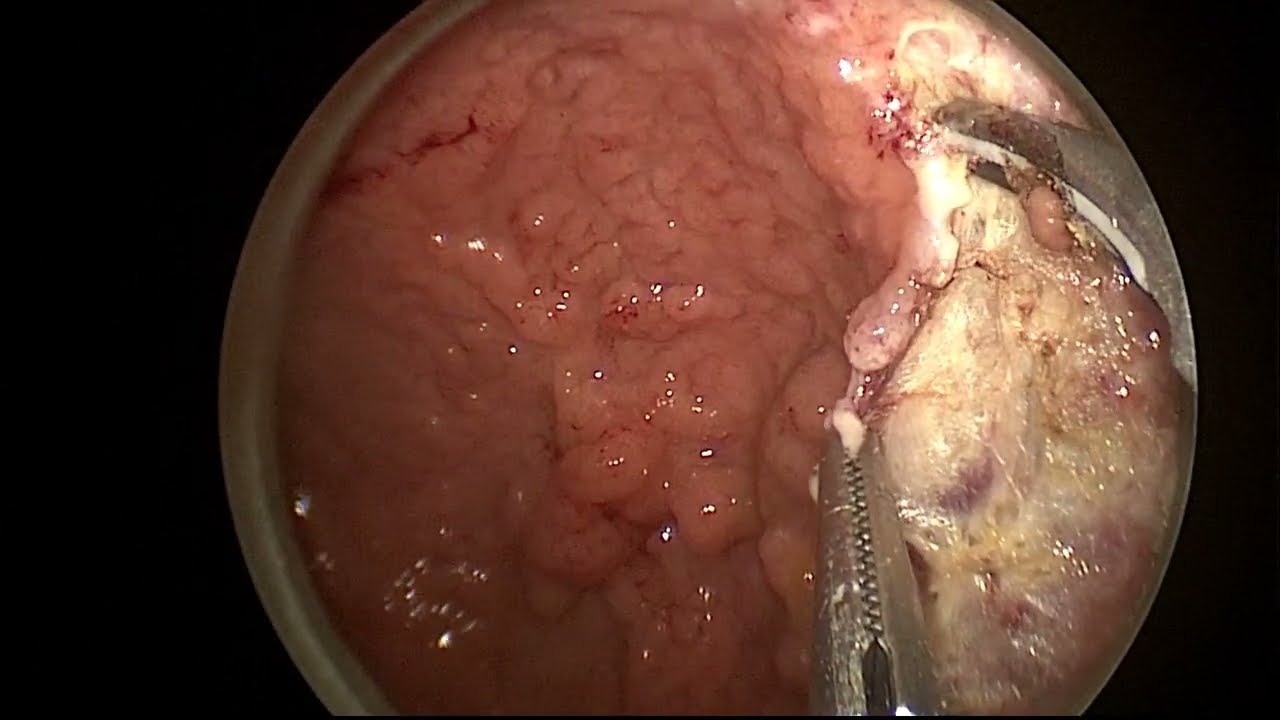
See how robotic colorectal surgery patients, just like you, returned to everyday life.



Dr. Mark grew up in Durban and matriculated in the top 30 in Natal. He completed his medical undergraduate training at UCT in 1998, where he was the elected class rep. for five years. He won the Family Medicine class medal, and Frank Foreman prize for the greatest contribution to student affairs. Internship at Edendale Hospital in Pietermaritzburg was followed by a year at various secondary hospitals in Cape Town for his community service, and then a year getting some GP experience in Manitoba, Canada. In 2002 Mark returned to Cape Town to specialise in general surgery at UCT. He completed this training in 2006, being awarded the ASSA prize for surgical research, and the Swann-Morton prize for the best surgical registrar.
Super-specialist training in HPB (Hepato-Pancreatico-Biliary) surgery started with the 2-year Certificate in Surgical Gastroenterology at Groote Schuur Hospital, with the CMSA exams completed at the end of 2008. In 2009 Mark further expanded his HPB experience and training with a Fellowship in HPB surgery at the HPB/Transplant unit in Newcastle-upon-Tyne, UK.
Super-specialist training in HPB (Hepato-Pancreatico-Biliary) surgery started with the 2-year Certificate in Surgical Gastroenterology at Groote Schuur Hospital, with the CMSA exams completed at the end of 2008. In 2009 Mark further expanded his HPB experience and training with a Fellowship in HPB surgery at the HPB/Transplant unit in Newcastle-upon-Tyne, UK.
Mark joined the Matley and Partners team in 2010. His primary interest is in HPB surgery, and he is accomplished in all aspects of this discipline, ranging from the management of gallstone disease, to complex liver and pancreatic resections. He is a keen endoscopist, including gastroscopy, colonoscopy and ERCP. Mark was the first surgeon in South Africa to perform the ALPPS liver resection procedure. In addition to the HPB surgery, Mark enjoys all aspects of general and laparoscopic surgery, including laparoscopic hernia repairs. He is a believer in team work, and tries to blend the best of modern techniques and technology with some old-fashioned “good bed-side manner”, in addition to careful decision-making and surgical technical expertise.
Mark is married to Tanya and they have two children. Mark’s hobbies include golf, fly-fishing, and scuba diving. Despite more than 25 years in the Cape, he remains a Sharks fan.
Ebrahim joined the Matley Partnership as a specialist colorectal surgeon with international training in laparoscopy from both Amsterdam and Nottingham. He is a Capetonian who matriculated from Livingstone High School, and completed his MBChB at UCT in 2002.
He completed his internship in Durban, where he met his wife Khatija, and completed his community service in Khayelitsha, including an additional year there with Medicin Sans Frontier, rolling out their antiretroviral program.
After two years of surgery in the UK, he completed his specialist training in Cape Town, obtaining his FCS in 2013. During this time he was awarded the MMed degree from UCT for his dissertation “Systems delays in Breast Cancer”. He gained a broad experience in general surgery before two years of sub-speciality training in the colorectal unit at Groote Schuur. In 2016 he was awarded the Specialist Certificate in Surgical Gastroenterology.
In 2017, he was awarded the SASES travelling fellowship to work with internationally renowned colorectal and laparoscopic surgeon, Professor Willem Bemelman, at the Amsterdam Medical Centre. Thereafter he completed his year abroad as a colorectal fellow, in Nottingham, UK. This is a busy unit with 10 colorectal surgeons providing the full range of colorectal specialist services. During this time he gained invaluable experience in advanced laparoscopy for inflammatory bowel disease and cancer surgery, which are his specific interests, and he is currently accruing UK robotic credentialing. Ebrahim is one of a handful of accredited specialist colorectal surgeons in the Western Cape, adding this expertise to the GIT team at Matley and Partners.
He is married to Khatija, a full time Obstetrician & Gynaecologist consultant at Groote Schuur Hospital, and they have two children. He is a golfer, family man and enjoys travelling at home and abroad.


Dr. Henri Pickard is a specialist Vascular Surgeon who proudly continues a rich family tradition of surgical practice, following in the footsteps of both his grandfather and father. He studied Medicine at the University of Cape Town (UCT), beginning a journey deeply rooted in heritage and excellence.
After completing his internship in Pietermaritzburg and community service in East London, Henri developed a strong interest in surgery. In 2012, he returned to Cape Town to work at the Trauma Centre at Groote Schuur Hospital, followed by a period at Victoria Hospital where he gained a wide range of surgical experience.
In 2014, Henri began his MMed degree and specialist training in General Surgery at Groote Schuur Hospital through UCT. In 2020, driven by a passion for the precision and complexity of the field, he pursued sub-specialist training in Vascular Surgery.
Henri is known for his collaborative work in multidisciplinary teams, his commitment to achieving the best outcomes for his patients, and his compassionate, patient-centred approach.
He grew up in Pietermaritzburg, George, and Cape Town, and matriculated from Rondebosch Boys’ High School. A proud South African, Henri is an enthusiastic Two Oceans runner, avid cricket follower, passionate Springbok supporter, and a devoted follower of Jesus. He is also a committed family man, deeply devoted to his wife Tricia and their three young children.
Neil grew up in Worcester and matriculated from Esselen Park High School in 1985. He completed his medical training at the University of Cape Town in 1991 and did his internship at Livingstone Hospital in Port Elizabeth. Following internship Neil worked at Red Cross Children’s Hospital as a medical officer in paediatrics before joining Mitchells Plain community health centre, where he gained extensive experience in general medical practice. His surgical experience started in 1996 at Worcester Regional Hospital where he worked as a medical officer in General Surgery for 3 years, prior to starting his specialist surgical training at Groote Schuur hospital in 1999.
On completion of his training in general surgery he was appointed as a consultant general surgeon at New Somerset hospital in 2005, where he was responsible for all clinical services until 2007 when he started his sub-specialist training in vascular surgery at St James’s hospital, the academic hospital of Trinity College Dublin in the Republic of Ireland. During his 3 year training period in vascular surgery, Neil received expert training in all aspects of open, endovascular and venous surgery at this prestigious high case volume unit. Neil returned to Cape Town in 2010 and was appointed as a consultant vascular surgeon at Groote Schuur hospital. In 2014 he was appointed as head of the vascular unit at University of South Africa (Medunsa) in Pretoria.
During the past 7 years, he was responsible for undergraduate, postgraduate and fellowship vascular teaching and training at the university as well as doing private practice at Netcare Unitas hospital in Centurion. Neil has served on the EXCO of the Vascular Society of South Africa since 2014.
Neil is an accomplished and experienced vascular surgeon, with special interests in endovascular surgery, dialysis access and venous surgery. He believes that good clinical practice is built on the foundation of empathetic bedside manner and teamwork.
Neil is married to Tracy, and they have 3 children. Neil enjoys an active outdoor lifestyle with hobbies including running, cycling, and golf. He also has a keen interest in history and philosophy.
Philip Matley has been a vascular surgeon in the practice that now bears his name since 1990. He is past-President of the Vascular Surgery Society of South Africa and a past moderator and chief examiner for the vascular surgery specialist examinations in South Africa. He has served on various national and international regulatory bodies and educational foundations.
During his training in Cape Town, he was the recipient of numerous awards including the Douglas Medal for the best candidate in the examination for the Fellowship of the College of Surgeons of South Africa as well as the Phyllis Knocker-Bradlow Award.
He has a special interest in the minimally invasive treatment of varicose veins, improving the circulation in the legs and brain through stents or surgery and the treatment of aneurysms.
In addition to his surgical practice, he is the chairman of Surgicom, the management body for private surgery practice in South Africa and serves on the board of South African Private Practitioners Forum (SAPPF).
Philip Matley grew up in KZN and is a keen golfer, mountain biker, walker and traveller